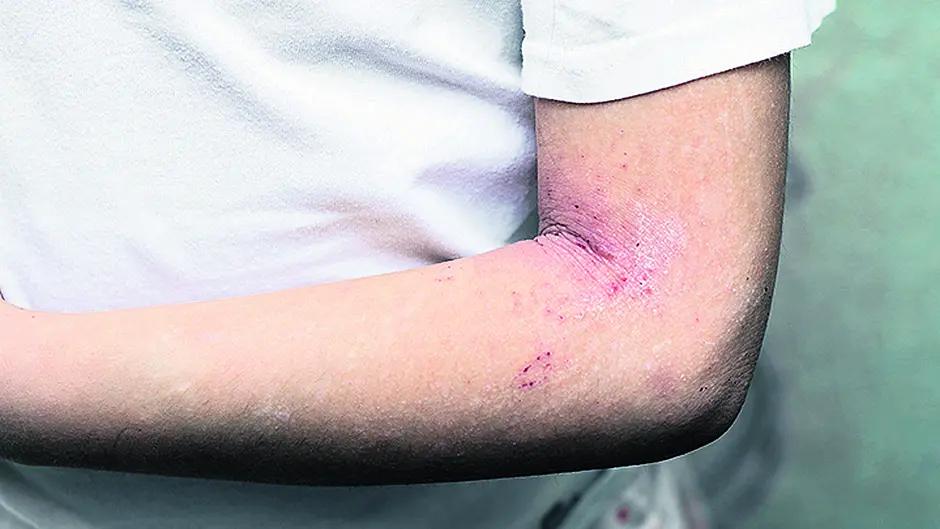
Global Eczema Day, which takes place next week, brings into focus a condition that affects around one in five under six-year-olds and one in 12 adults.
By Rosie Shelley
GLOBAL Eczema Day, which takes place next week, brings into focus a condition that affects around one in five under six-year-olds and one in 12 adults. And it’s rising all the time, in line with all allergic conditions, partly because of what’s being called the ‘hygiene hypothesis’: we are now so obsessed with killing germs that our babies are simply not being exposed to enough bacteria for the proper development and functioning of their immune systems.
This chimes with research from last year showing that children born into homes with dogs gain protection from developing the condition.
We’ve always been aware that eczema is an inflammatory condition, with a strong genetic component, but we know now that it is in fact an autoimmune disorder. Meaning that the immune system gets out of kilter and the body mistakenly attacks its own tissues. We’re increasingly coming to understand the domino effect of intestinal bacteria on the immune system (which is largely based in the gut), autoimmune diseases, allergies and all forms of chronic inflammation.
Antiobiotics
This gut bacteria link was underlined when a study found that babies given antibiotics (which kill off good bacteria as well as bad) in their first year were a full 40% more likely to develop eczema. Conversely, another study supplied the lactobacilli probiotic to newborns with a genetic predisposition, and found them half as likely to develop the condition. Similar results were achieved by giving the bacteria to pregnant women with a family history. Patients taking a probiotic have experienced huge improvements in their skin, and in some cases no further return of symptoms. This year, scientists have been working on using the bacteria from healthy skin in a topical fashion. And separately, it was discovered that pregnant women who take fish oils (highly anti-inflammatory), and probiotic supplements reduce their child’s risk of both eczema and food allergy.
Stress can trigger
For healthy intestinal balance we also need healthy fats, and sufferers have been found to have a faulty fat metabolism and/or deficiency in essential fats. Food allergies are often implicated. And we know that stress plays a huge part in flare ups, probably because stress hormones unbalance the immune response and increase inflammatory markers.
There are of course medical options for the treatment of eczema, and they may be necessary in severe cases, but each of them carries side-effects. Steroid creams, for example, can cause skin thinning, and (because they suppress immune function) leave broken skin very vulnerable to infection. Those infections will likely be treated with antibiotics, which of course further knock out the vital gut bacteria, and so it goes. And a word about the aqueous cream BP that was traditionally recommended — it contains SLS which also thins the skin, and irritates and damages its natural protective barrier in as little as four weeks. As is so often the case, what’s needed here is a multi-faceted approach:
1. Boost levels of good bacteria. Take a probiotic supplement that contains the acidophilus strain, such as Bio Kult. Eat prebiotic foods (onion, garlic, leek, celery, asparagus, artichokes, bitter leaves, lentils, root veg, bananas) every day.
2. Avoid things that disable the action of good gut bacteria or feed the bad: sugars and artificial sweeteners, white grains, unnecessary antibiotic use, antibacterial mouthwashes and soaps. Alcohol in these strips the skin of its protective barrier, while the active ingredient triclosan, also found in some face washes, deodorants, toothpastes etc has been proven to interfere with good gut bacteria. And it’s a hormone disruptor.
3. Eat plenty of anti-inflammatory essential fats from oily fish and olive oil. Introducing fish soon after weaning can slash the incidence of eczema by a quarter. Nuts lower levels of the inflammatory markers involved in autoimmune reactions, while increasing levels of good gut bacteria by 8%.
4. Establish what, if any, food allergies or intolerances you might have by keeping a food and symptom diary. The most common in people with eczema are dairy, eggs, peanuts, wheat, soya and citrus.
5. Avoid inflammatory foods and drinks eg sugars and white grains, seed oils such as sunflower oil, processed food, fizzy drinks, and trans/hydrogenated fats. In July a large study confirmed a strong link between eczema rates and the amount of junk food a child eats.
6. Include plenty of anti-inflammatory, antioxidant (brightly coloured) vegetables, oily fish, turmeric and ginger, green tea.
7. Avoid man-made fibres, commercial cleaning products, perfumes and toiletries containing long lists of chemicals, especially skin-irritating SLS or SLES—buy them from the healthfood shop and look for natural ingredients like shea butter, calendula, vitamin E, almond oil, coconut oil and chamomile, or brands such as Lavera, Aveeno Dermexa, Green People, Eucerin, and E45. Use non-bio washing powder.
8. Vitamins C, D and E, magnesium, zinc, omega-3 oils and the antioxidant quercetin are all involved in counteracting the allergic response, and people with eczema have variously been found to be deficient in most of them. Supplement, and/or eat plenty of greens, onions and garlic, olives, butternut squash, asparagus, celery, berries and cherries, apples, non-wheat wholegrains especially buckwheat, lentils, organic meat and poultry, and again if not allergic oily fish. Children should be supplemented with vitamin D3 and exposed to a little sunshine—those in colder climates are twice as likely to develop the disorder. Recent research also suggests that children whose mothers had higher levels of vitamin B3 (B complex, animal and fish proteins, nuts) in pregnancy have a lower risk.
9. Infants with a limited variety of gut bacteria were found to have a significantly higher incidence by 18 months. Women planning a vaginal birth (which is how the child picks up the good bacteria) should eat fermented/aged foods like sauerkraut, hard cheeses, sourdough bread and live yoghurt.